Pain and the immune-system
In one of the latest CRAFTA Blogs my lovely colleague Gemma from beautiful Barcelona was writing about Bruxism and how to interpret, assess and treat this condition.
In one of the latest CRAFTA Blogs my lovely colleague Gemma from beautiful Barcelona was writing about Bruxism and how to interpret, assess and treat this condition. She perfectly described the important role of clinical reasoning processes when treating patients with several problems like pain and movement dysfunction or symptoms like dizziness or tinnitus. Gemma referred to Louis Gifford’s Mature Organism Model, which is not just a very clever system to understand pain mechanisms, but also to use it as therapeutic tool for patient education.
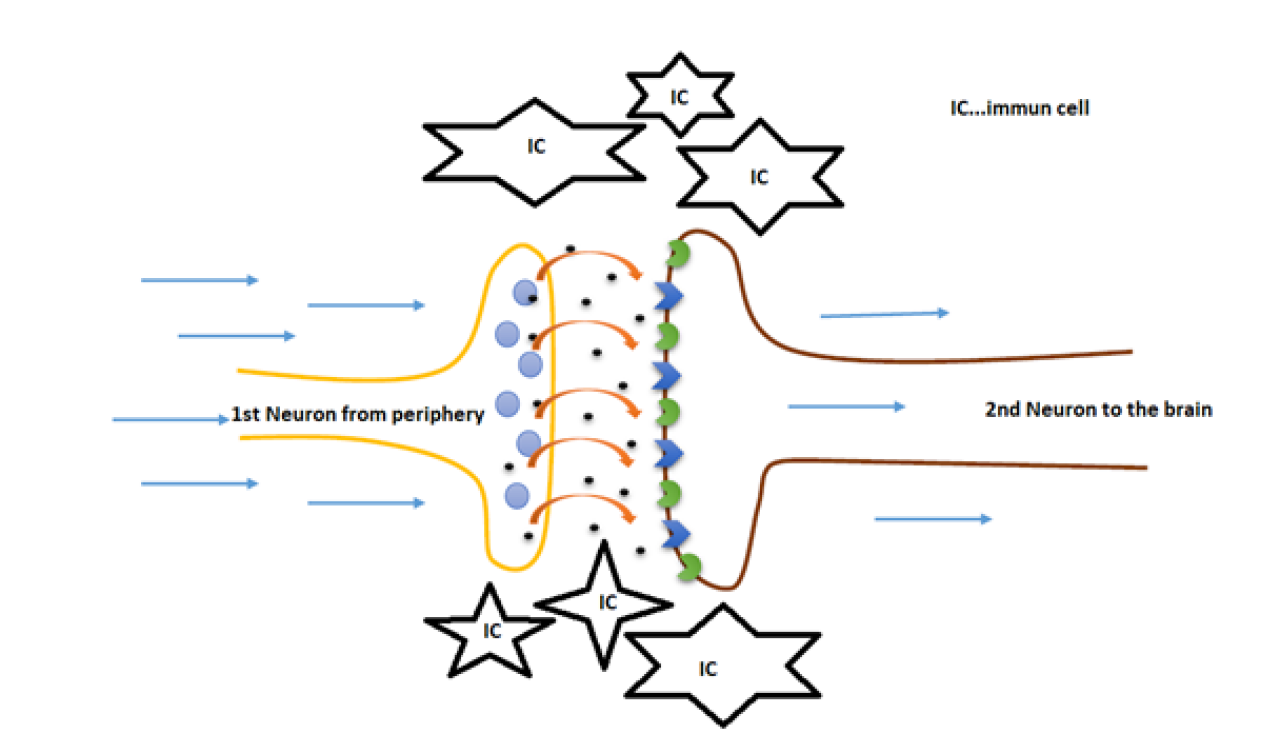
Gifford described a cycle of INPUT – SCUTINISING – OUTPUT that is able to facilitate itself, and is also under certain external influence, as it might be stress or other emotional situations. But there are not just certain external factors that are able to influence the peripheral and central processing of pain disorders. Since several years, scientists come up with lots of data to the role of the humans´ immune system on pain and other, quite complex, diseases.





